A truly successful hospital project is a masterful blend of clinical precision and human-centric design. It's about creating a space that not only heals patients but also empowers staff and delivers a solid return on investment. This isn't just about architecture; it's about understanding how every wall, window, and workflow directly impacts everything from infection rates to the bottom line.
The Strategic Blueprint for Successful Hospital Design
Think of a hospital less as a building and more as a complex, living ecosystem. For any developer or owner, the smartest move is to treat it as a high-performance asset right from the drawing board. Every single design choice, whether it's the overall campus layout or the exact placement of a hand sanitizer dispenser, has long-term consequences. These decisions echo for decades, influencing patient recovery, staff burnout rates, and the facility's financial health.
This mindset shifts architecture from a simple cost center to a core value driver. When a hospital is designed with intention, it just runs better. Nurses walk fewer miles per shift, and patient flow through high-traffic areas like the emergency department becomes smoother. A key goal is to embed strategies to boost hospital operational efficiency right into the physical DNA of the building.
Pillars of High-Performance Hospital Design
From my experience, every great healthcare facility is built on three pillars. They are completely intertwined—if one is shaky, the whole structure suffers. The real art is designing a building where architectural choices produce measurable, positive results in all three areas.
-
Improved Patient Outcomes: This is all about creating a healing environment. It’s amazing what simple design choices can do. Things like maximizing natural light, designing for quieter corridors, and ensuring a patient can easily find their way around have been proven to lower stress, reduce the need for pain medication, and actually shorten hospital stays.
-
Enhanced Operational Efficiency: A smart layout is a game-changer for staff. By cutting down on how far they have to walk for supplies or to get to a patient, you eliminate workflow bottlenecks. This means clinicians can spend less time running around and more time on what matters: patient care. The impact on operational costs is immediate and significant.
-
Strong Financial ROI: When you improve patient outcomes and boost efficiency, the hospital naturally becomes a more profitable, sustainable asset. It becomes a place that attracts and retains the best medical talent, earns higher patient satisfaction scores, and cements its reputation as a leader in the community.
This diagram really brings home how these core pillars support any successful hospital project.
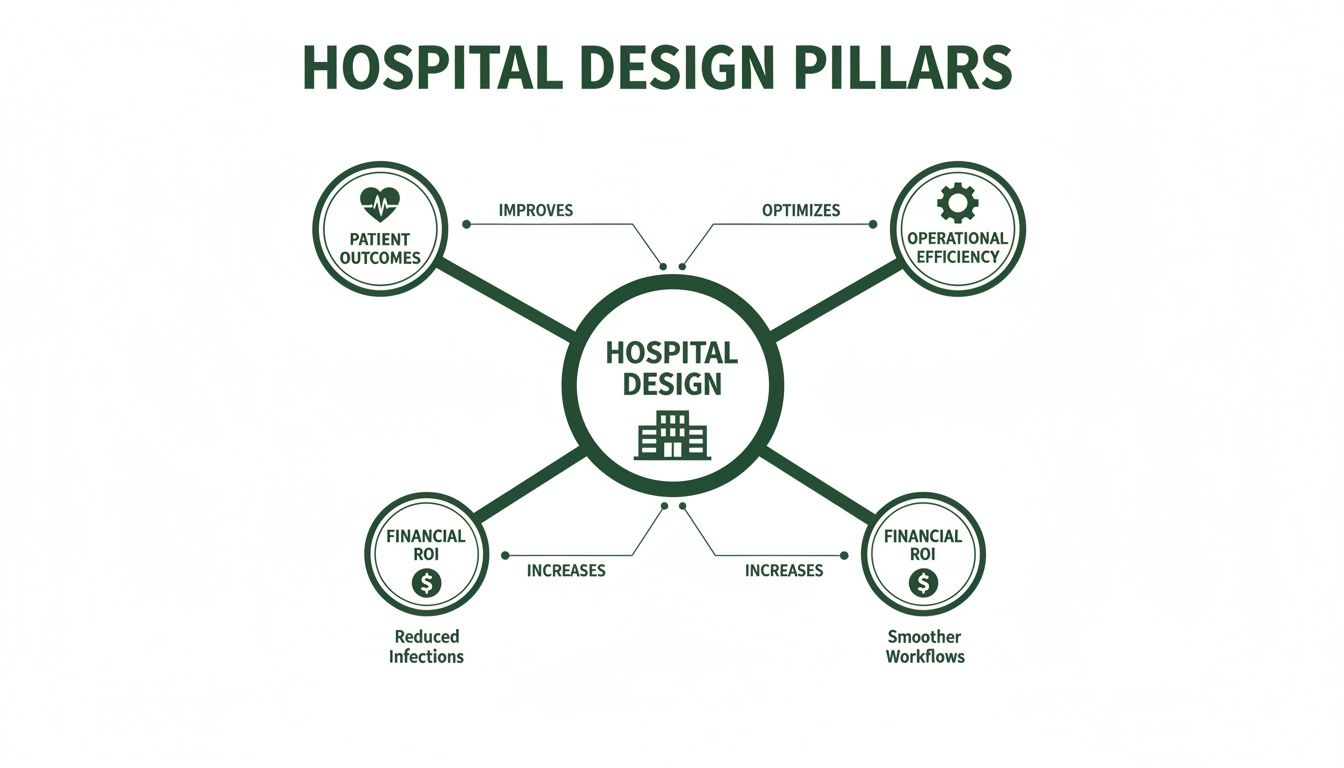
As you can see, patient outcomes, operational efficiency, and financial return are not separate goals. They're all connected, with thoughtful design acting as the foundation that holds everything together.
Mastering Site Planning for Future-Proof Hospitals
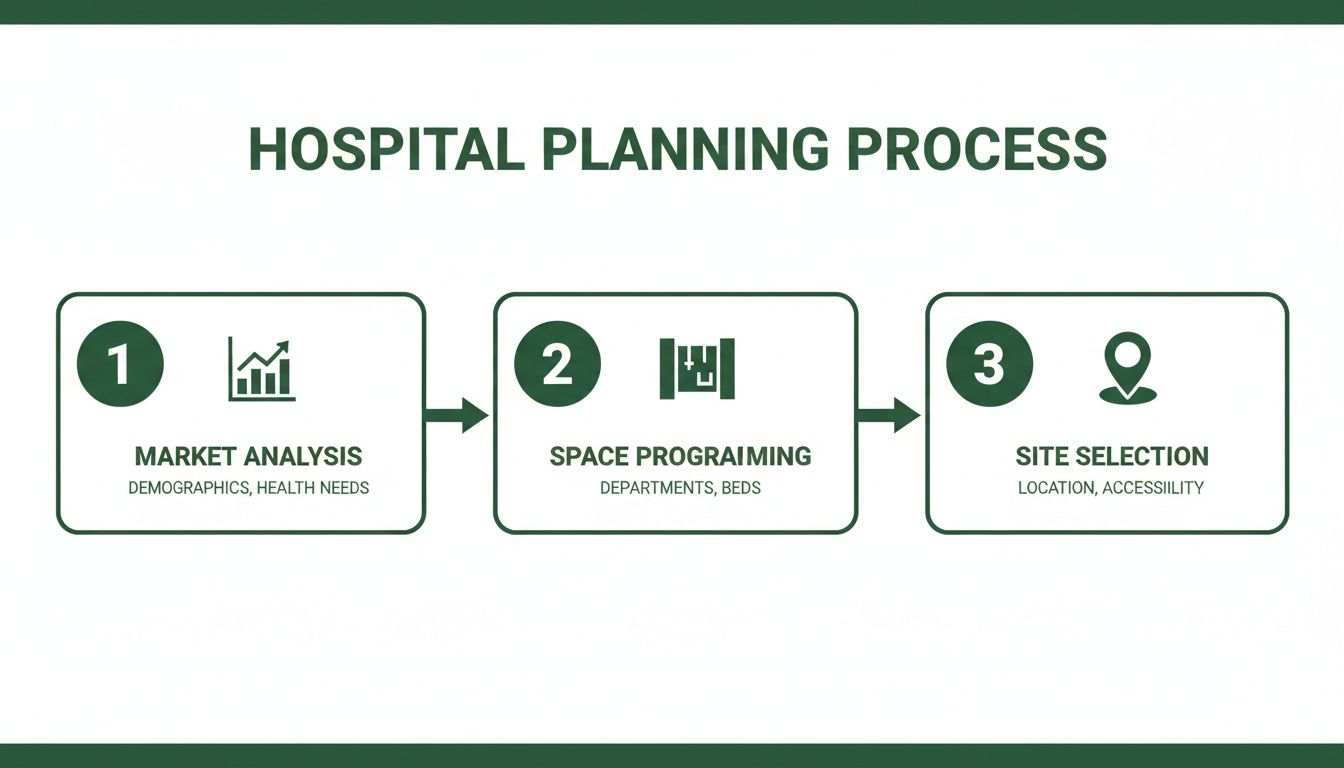
The success of a new hospital is often decided long before the first shovel hits the dirt. Strategic site planning isn't just a preliminary step; it's the very foundation of the entire project, shaping everything from patient access and emergency vehicle routes to the hospital's ability to expand down the road. It’s the single most important part of the design for hospital process.
Think of a hospital campus less like a single building and more like a small, highly specialized city. Its success depends entirely on a well-designed road grid. When the Emergency Department has a straight shot to Radiology and the Surgical Suites, you shave off precious minutes, boost efficiency, and directly improve patient outcomes. On the flip side, poor planning creates permanent operational headaches that will cost time, money, and potentially lives for decades.
This is the phase where we, as developers and architects, really dig into a potential site's DNA. The mission is to ensure the property can handle not just the hospital we need today, but also the inevitable growth and technological shifts of the next 20 or 30 years.
Core Factors in Hospital Site Evaluation
Choosing the right spot is a balancing act, weighing community needs against the hard realities of logistics and regulations. Simply finding enough available acreage isn't nearly enough.
A thorough analysis always looks at a few key factors:
- Community and Demographic Analysis: Is the site actually where patients need it? We have to look at population density, growth projections, and accessibility via major roads and public transit for patients and staff alike.
- Zoning and Land Use: You can't fight city hall. Navigating local ordinances is non-negotiable, so an ideal site is either already zoned for medical use or has a clear path to getting rezoned. This helps avoid long, expensive approval battles.
- Topography and Environmental Conditions: A relatively flat site is a gift, saving a fortune in excavation costs. We also have to vet things like soil stability and flood risk to head off major structural problems later on.
Getting this foundational data right from the start helps us make an informed decision. Skipping over any one of these can inject massive risk and unforeseen costs into the project.
A hospital's physical location is its first promise to the community it serves. A well-chosen site says, 'We are here for you, easy to reach in a crisis, and ready to grow with your needs.'
Planning for Today and Tomorrow
Once a solid site is in our sights, the focus shifts to the master plan. This is where we need to balance immediate operational needs with long-term flexibility. A little strategic foresight here can save millions in renovation costs later.
A smart master plan has to nail several critical flows:
- Emergency Access: First and foremost, you need clear, unimpeded routes for ambulances. This entrance has to be completely separate from the main public entrance to prevent bottlenecks during a crisis.
- Public and Patient Flow: The main entrance should feel welcoming and be simple to navigate. We need intuitive wayfinding to key departments and plenty of accessible parking.
- Service and Supply Logistics: Behind the scenes, a dedicated service entrance is essential for deliveries, waste removal, and maintenance. This keeps the backstage operations from ever interfering with patient care.
- Future Expansion Zones: The layout must intentionally set aside land for future wings, new service lines, or extra parking structures. Crucially, this has to be planned so that future construction won't disrupt the existing hospital.
This level of detailed planning shows just how much is at stake. The global healthcare architecture market was valued at USD 8.89 billion and is expected to hit USD 13.21 billion by 2032. For developers in the U.S., where design-build is projected to account for 47% of construction spending by 2028, getting the site plan right is the most effective way to secure a return on this massive investment. You can see more on these trends in the latest industry report from Fortune Business Insights.
Designing for Patient Safety and Infection Control
When you're designing a hospital, the architectural decisions you make aren't just about aesthetics or efficiency—they're a matter of life and death. The physical layout of a building can either be your strongest ally in fighting infection or a hidden liability that puts patients at risk. Getting this right is non-negotiable; it's the foundation of any successful healthcare project and directly impacts patient outcomes and the hospital's reputation.
The first step is to think about workflows like a one-way street system designed to prevent collisions. We apply that same logic by creating completely separate “clean” and “dirty” pathways. This isn't just a suggestion; it's a critical strategy to keep sterile supplies from ever crossing paths with used materials or waste, preventing the spread of dangerous pathogens from a soiled utility room to, say, a sterile operating theater.
Building Defenses Against Infection
Stopping hospital-acquired infections (HAIs) requires weaving a multi-layered defense system right into the building's DNA. This goes so much deeper than just good cleaning routines. It’s about creating an environment that is fundamentally hostile to germs.
Here are a few of the most critical design strategies we use:
- Ventilation and Airflow: You absolutely cannot skimp on specialized HVAC systems, especially in high-risk areas. For instance, negative-pressure isolation rooms are engineered so air flows into the room from the corridor but can’t escape back out. This traps airborne contaminants inside, protecting everyone else in the hospital.
- Material Selection: Surfaces are the front lines in the war on germs. We have to specify materials for floors, walls, and counters that are non-porous, incredibly durable, and easy to sanitize. Even tiny details matter, like minimizing seams and joints where microbes love to hide.
- Spatial Separation: Sometimes the simplest solution is the best. Just providing enough space between patient beds makes a huge difference. In fact, single-patient rooms are now the gold standard because they dramatically reduce infection transmission and, as a bonus, let patients rest better.
Beyond powerful ventilation, it’s our job to embed proven principles for preventing cross-contamination into every aspect of the layout. Every single choice, from the type of door handle to the finish on the walls, is an opportunity to make the building safer.
The Healing Power of Evidence-Based Design
But patient safety is more than just fighting infections. The physical environment itself has a real, measurable effect on a patient's mental state, which in turn speeds up—or slows down—their physical recovery. This is the whole idea behind evidence-based design (EBD), a practice that uses solid research to create spaces that actively help people heal.
A healing environment isn't a luxury; it's a clinical tool. Thoughtful design can reduce patient anxiety, lower the need for pain medication, and even shorten the length of a hospital stay, delivering clear returns for both the patient and the provider.
For developers and owners, thinking about EBD isn't an expense; it’s a strategic investment in better outcomes. The key elements are surprisingly straightforward:
- Maximizing Natural Light: Sunlight isn't just pleasant; it helps regulate a patient's circadian rhythms, leading to better sleep and less depression. Time and again, studies have shown that rooms with large windows and views of nature lead to faster recovery times.
- Clear Wayfinding: Nothing raises stress levels faster than getting lost in a sprawling, confusing hospital. Intuitive signage, logical floor plans, and memorable landmarks are essential to help anxious patients and visitors navigate with confidence.
- Acoustic Control: Hospitals are notoriously noisy, and all that racket is a major stressor. Using sound-absorbing materials and designing quieter nurse stations and corridors creates a much more restful, therapeutic atmosphere for everyone.
By weaving these principles into the design from day one, a hospital becomes more than just a place to get treated. It transforms into an active partner in the healing process—a facility that not only safeguards patients but also protects its own operational integrity for years to come.
Integrating Complex MEP and Technology Systems

If a hospital's structure is its skeleton, then the Mechanical, Electrical, and Plumbing (MEP) systems are its vital organs and central nervous system. These intricate networks are the facility's lifeblood, humming away behind the walls to make sure patient care happens without a hitch. For developers and owners, getting a handle on this complexity is non-negotiable for a successful design for hospital project.
Think of the hospital as a living, breathing thing. Its electrical grid is the nervous system, powering everything from life-support machines to the surgeon's overhead light. The plumbing and medical gas lines act as the circulatory system, pushing clean water, oxygen, and vacuum pressure exactly where they need to go. And the HVAC system? That's the lungs, constantly circulating clean, filtered air while whisking away contaminants.
This isn't just a clever analogy—it's the reality of the stakes. A failure in any one of these systems can have immediate, life-threatening consequences. That’s why intelligent, coordinated MEP planning isn't just a technical box to check; it’s a core part of risk management and building a truly resilient facility.
Coordinating Mission-Critical Infrastructure
Seamless integration is the name of the game. In a hospital, the MEP and technology systems are light-years more complex than in your typical office building. They have to work together in a tightly choreographed dance, and it’s the architect’s job to act as the conductor for a massive team of engineers and specialists.
Several areas require absolute precision:
- Redundant Power Systems: A hospital simply cannot lose power. Period. The design has to include multiple layers of backup, from uninterruptible power supplies (UPS) for instant, momentary support to massive generators capable of running the entire facility for days.
- Specialized HVAC Requirements: An operating room has drastically different air filtration and pressure needs than a public waiting area. The HVAC system must be meticulously zoned to serve the specific clinical demands of each space, preventing cross-contamination and maintaining sterile fields.
- Medical Gas Distribution: A dedicated, and highly regulated, network of pipes is needed to safely deliver oxygen, medical air, and vacuum suction. The layout has to be perfect—planned for safety, efficiency, and easy access for future maintenance.
- Robust Data Infrastructure: Modern medicine runs on data. The building must support a huge network of cabling for electronic health records (EHR), diagnostic imaging, patient monitoring systems, and secure Wi-Fi for both staff and visitors.
The biggest headache is preventing system clashes. Without one person leading the charge, you'll inevitably find a plumbing line routed through the exact same space an HVAC duct needs to occupy. An experienced architect spots these conflicts before they happen, saving immense time and money while ensuring all systems fit together and can be easily maintained later on.
A well-designed MEP system is invisible when it works perfectly but catastrophic when it fails. The architect's role is to ensure its invisibility by orchestrating a flawless integration from day one.
The Architect as System Integrator
Ultimately, the architect is the one responsible for turning a dozen independent systems into a single, high-performing whole. This leadership is what keeps a project on track and on budget, all while making sure the finished building meets every operational and regulatory standard.
The architect’s role in MEP coordination is multifaceted. They become the central hub of communication between mechanical, electrical, plumbing, and structural engineers, ensuring the needs of one system don't compromise another.
They also have to think about the future. This means designing systems with enough spare capacity for the medical technologies of tomorrow. It also means planning for interstitial spaces—the valuable real estate between floors—to allow for easier maintenance and upgrades down the line without shutting down critical hospital operations. A smart design for hospital MEP strategy is truly the cornerstone of an efficient, resilient, and safe healthcare environment.
The following table breaks down the core MEP systems and the specific challenges they present in a hospital setting.
Key MEP System Considerations in Hospital Design
| MEP System | Primary Function in Hospital | Key Design Challenge |
|---|---|---|
| HVAC | Controls air temperature, humidity, filtration, and pressure to prevent infection spread and maintain sterile environments. | Meeting diverse and strict air change rates (ACH) and pressure relationships for different clinical zones (e.g., ORs vs. patient rooms). |
| Electrical Power | Provides reliable normal and emergency power to all equipment, from lighting to critical life-support machines. | Designing robust and redundant power sources (generators, UPS) with seamless, automatic transfer to avoid any interruption in care. |
| Plumbing | Delivers potable water, hot water, and manages sanitary and storm drainage. Includes specialized systems for medical waste. | Ensuring proper backflow prevention, managing high water demand, and designing specialized drainage for labs and treatment areas. |
| Medical Gas Systems | A dedicated piping network that delivers life-sustaining gases like oxygen, medical air, nitrous oxide, and vacuum suction. | Ensuring 100% system integrity and safety through meticulous planning, installation, and rigorous testing to prevent leaks or cross-contamination. |
| Data & Technology | Supports electronic health records (EHR), nurse call systems, patient monitoring, imaging (PACS), and building automation. | Planning for massive cable pathways, secure network closets, and sufficient bandwidth while future-proofing for next-gen technologies. |
Each of these systems is a project in itself, but in a hospital, they must function as one cohesive, reliable unit.
Navigating Healthcare Codes and Regulations

For any developer or owner new to the healthcare space, the sheer volume of codes and regulations can be intimidating. It often feels like the biggest roadblock in a design for hospital project—a confusing mix of acronyms and rules that seem built to cause delays.
The best way to approach this isn't to see these codes as obstacles, but as a roadmap. Every rule, from a local building code to a federal accessibility standard, is there for a critical reason: to keep patients and staff safe and ensure the facility operates as it should. Tackling compliance head-on from the very first design meeting isn't just a good idea; it's the only way to manage risk and keep a project on track.
This is where having an experienced architectural partner becomes invaluable. They’ve been down this road before. They know how to spot regulatory pitfalls early, translate dense code requirements into practical design decisions, and ultimately, guide the project through the approvals process without costly surprises.
Understanding the Key Governing Bodies
While you’ll deal with plenty of local and state authorities, a handful of major players establish the standards that influence nearly every healthcare project in the U.S. Knowing who they are and what they do is the first step.
You’ll run into these primary groups constantly:
- Facility Guidelines Institute (FGI): Think of the FGI Guidelines as the foundational rulebook. They set the minimum standards for almost everything, from the square footage of an operating room to the types of materials you can use on the walls in patient areas. Most states adopt these guidelines as their baseline.
- Americans with Disabilities Act (ADA): The ADA is about ensuring everyone has equal access. In a hospital, this means much more than just ramps and parking spots. It dictates corridor widths for gurney turning radiuses, clearances needed for patient lifts, and even how easy it is for someone in a wheelchair to use a sink or call button.
- State Health Departments: Every state has its own health department that licenses and approves hospital construction. They typically start with the FGI Guidelines but almost always add their own unique—and often stricter—requirements.
This is why it's so important to work with a design team that has a strong track record in your specific state. Their local knowledge can save you from having to do expensive redesigns after the first round of plan reviews.
Think of healthcare codes as the "rules of the road" for hospital construction. You wouldn't build a highway without them, and you can't build a safe, licensable hospital without a deep understanding of the regulatory framework.
The Role of Proactive Planning and Documentation
The secret to a smooth regulatory journey is getting ahead of it. Don't wait for a plan reviewer to send back a list of corrections. A smart project anticipates what reviewers are looking for and builds a solid compliance strategy right into the earliest design sketches.
This means documentation can't be an afterthought; it has to be a core part of the process. Every drawing and specification is proof that your design meets all the non-negotiable requirements for life safety, infection control, and patient access.
An architectural team that specializes in healthcare will assemble this evidence meticulously, making the trip through the approvals pipeline far less painful. By taking this proactive stance, you can move forward with confidence, knowing you're building a facility that will be fully licensable from day one. It transforms a potential bottleneck into a predictable, manageable part of the project.
Giving Old Buildings New Life: The Rise of Adaptive Reuse in Healthcare
The old playbook for expanding healthcare services—finding an empty plot of land and building a massive new hospital from the ground up—isn't the only option anymore. In fact, a smarter, more nimble strategy is taking hold: adaptive reuse. This is the art of transforming existing, often overlooked buildings into state-of-the-art medical facilities.
Think of it this way: instead of starting from scratch, your raw material might be an old, shuttered big-box store or a half-empty office building. It’s a story of transformation, one that shows savvy developers and healthcare owners how to unlock the incredible potential hiding in plain sight. By giving an existing structure a new and vital purpose, you're not just building a clinic; you're breathing new life into a community asset.
This isn't just a passing trend; it's a fundamental shift in how the industry thinks about growth. Within the broader design for hospital sector, renovation and adaptive reuse now go toe-to-toe with new greenfield campuses for investment dollars. The healthcare architecture market in the U.S. alone is on track to hit USD 2.79 billion by 2030.
Look at the numbers from a recent survey: while 34% of facilities were planning new or expanded hospitals, a nearly equal number were focused on infrastructure upgrades (18%) and central plant projects (17%). Medical office buildings (MOBs), which are often perfect for reuse projects, continue to be a hotbed of activity. You can dig deeper into the numbers and see the durable opportunity in healthcare conversions for yourself.
Spotting the Right Candidates for Conversion
Not every empty building has what it takes to become a healthcare facility. The best candidates have "good bones"—a solid foundation that can support the intense demands of a clinical setting. Getting this right from the start makes the entire conversion process smoother and more financially sound.
Here are the types of buildings that often make for successful projects:
- Former Big-Box Retail Stores: These are goldmines for outpatient clinics or ambulatory surgery centers. Their massive, open floor plans, high ceilings, and acres of parking are huge assets. You can easily carve out space for clinical pods, waiting areas, and procedure rooms.
- Vacant Office Buildings: A multi-story office building can be a great fit for specialty clinics or a multi-tenant medical office building (MOB). While the existing electrical and plumbing will need a serious overhaul, they provide a solid framework to build upon.
- Underutilized Warehouses: Much like retail stores, warehouses offer vast, flexible spaces. They're especially well-suited for services that need room for bulky equipment, such as imaging centers or large-scale physical therapy facilities.
The Unique Hurdles of a Healthcare Conversion
While the benefits are clear, turning an old building into a modern medical center comes with its own set of challenges. This isn't a blank-slate project; it’s more like skillfully retrofitting a high-performance engine into the chassis of a classic car. You absolutely need an experienced architectural partner to navigate the inevitable twists and turns.
The art of adaptive reuse in healthcare is seeing past what a building was and envisioning what it can become. It's a puzzle of integrating advanced medical systems within an existing frame while honoring the building's original character.
You have to be ready to tackle a few key challenges head-on:
- Beefing Up the Structure and Infrastructure: Medical equipment—think MRI and CT scanners—is incredibly heavy. Floors often need to be structurally reinforced to handle the load. Then there's the complex web of MEP (Mechanical, Electrical, Plumbing) systems for medical gases, backup power, and specialized HVAC, all of which must be threaded through a structure that was never designed for them.
- Meeting Today's Strict Healthcare Codes: The entire building has to be brought up to modern healthcare codes, including the FGI Guidelines and ADA requirements. This can mean widening corridors, installing new fire suppression systems, and ensuring every finish meets exacting infection control standards—all within the constraints of an existing frame.
- Dealing with Hidden Hazards: Older buildings often come with baggage like asbestos or lead-based paint. These hazardous materials have to be completely and safely removed before any real renovation work can start, which adds a critical, and often costly, first step to the project.
By getting ahead of these issues, developers can turn a forgotten building into a vital community healthcare asset, delivering immense value in the process.
Common Questions on Hospital Design Answered
Diving into a hospital design project can feel overwhelming. For developers and owners, the path is filled with questions. Here, we tackle some of the most common ones with straightforward, experience-based answers to help you navigate your next healthcare project.
What Are the Biggest Cost Drivers in a Hospital Design Project?
The most significant costs in a hospital build are rarely the things you see. They're hidden within the walls and ceilings—the complex systems and intense regulatory requirements that keep a modern medical facility running safely.
MEP systems (mechanical, electrical, plumbing) are a huge chunk of the budget. We're not talking about your standard office HVAC. Hospital systems demand sophisticated air filtration, fully redundant power grids with massive backup generators, and specialized medical gas lines. Each of these comes with a serious price tag.
Then there's the medical equipment, which dictates major architectural choices. An MRI machine, for example, is incredibly heavy and requires not just significant structural support but also specialized radio frequency (RF) shielding built directly into the room. This isn't just an equipment purchase; it's a construction project in itself.
Finally, every surface and finish must meet strict infection control standards. This means specifying materials that are non-porous, highly durable, and easy to clean—all of which are more expensive than typical commercial-grade products. A skilled architect will find savings through smart planning and value engineering, but these core requirements are non-negotiable.
How Long Does a Typical Hospital Project Take?
While every project is different, a good rule of thumb for a moderately sized hospital is 3 to 5 years from the first conversation to opening day. It's a marathon, with each leg of the race just as important as the last.
Here's how that timeline usually breaks down:
- Programming & Schematic Design: This is the foundational stage where we define goals and sketch out the big ideas. It usually takes 6 to 9 months.
- Design Development & Construction Documents: We spend 12 to 18 months turning those initial concepts into a highly detailed set of blueprints.
- Permitting & Regulatory Review: Getting the green light from all the necessary agencies can take anywhere from 3 to 6 months, and sometimes longer in certain cities.
- Construction: The actual build-out is typically the longest phase, requiring 18 to 24 months or more, depending on the project's complexity.
Adaptive reuse projects can sometimes shave time off this schedule, but they come with their own risks—like discovering a surprise in the existing structure that needs to be fixed.
Evidence-Based Design isn't about chasing trends; it's about using solid research to create environments that are clinically proven to improve healing, reduce staff stress, and increase patient safety. It's a strategic investment in better outcomes.
What Is Evidence-Based Design and Why Does It Matter?
Evidence-Based Design (EBD) is about taking the guesswork out of architecture. It’s a disciplined approach where we use credible, data-backed research to make design decisions that have a direct, positive impact on patients and staff. It’s where the science of medicine meets the art of architecture.
This isn't just about creating a pleasant atmosphere. It's about using the physical environment as a tool for healing. For instance, countless studies have shown that patient rooms with large windows and views of nature can actually reduce the need for pain medication and shorten hospital stays. Another great example is using lighting systems that support the body's natural circadian rhythms, helping patients rest better and recover more quickly.
For a hospital owner, EBD is simply good business. It leads to better patient satisfaction scores, helps attract and retain top medical talent, and can even reduce the rate of medical errors. Ultimately, it’s a powerful investment in the facility's bottom line and its reputation for providing world-class care.
At Sherer Architects, LLC, we specialize in guiding developers and owners through every stage of complex commercial projects, including new construction and adaptive reuse for healthcare. We transform challenges into opportunities, delivering beautiful, enduring, and sustainable results. Learn how our expertise can maximize the value of your next project.