When we talk about the design of a hospital, we're not just talking about architecture. We're talking about a highly specialized discipline where every wall, window, and workflow has a direct impact on patient healing, staff effectiveness, and the facility's bottom line. The goal is to create a high-performance environment that marries clinical precision with a deeply human touch.
Modern hospital design is no longer about guesswork; it’s about using data to get better health outcomes, slash infection rates, and make the entire experience of giving and receiving care better for everyone involved.
The Blueprint for a Healing Environment

A hospital today is so much more than a building filled with medical gear. It’s a carefully orchestrated ecosystem built for one purpose: healing. The sterile, intimidating hallways of the past are giving way to spaces that feel welcoming, are easy to navigate, and actively contribute to recovery.
This whole shift is powered by a concept called Evidence-Based Design (EBD).
Think of EBD like a clinical trial for architecture. A doctor wouldn't prescribe a medication without solid research proving it works, right? In the same way, architects and developers now use hard data to make design choices proven to improve patient results. Every decision, from the view out a patient's window to the acoustics in a nurse's station, is backed by research showing it makes a real difference.
Key Pillars of Modern Hospital Design
A truly successful hospital design is built on three fundamental pillars. Get these right, and you create a facility that not only serves the community today but is ready for whatever comes next.
-
Patient Experience: This isn't just about comfy beds. It's about designing spaces that actively reduce stress, encourage rest, and empower patients. Things like single-patient rooms, plenty of natural light, and signage that makes sense aren't just nice-to-haves; they lead to higher satisfaction scores and measurably better clinical outcomes.
-
Operational Workflow: In healthcare, efficiency saves lives. A smart design streamlines the movement of staff, patients, and supplies. It’s about logical adjacencies that cut down on footsteps and flexible spaces that can easily adapt to a sudden influx of patients or the arrival of a new piece of medical technology.
-
Future-Proofing and Resilience: A hospital is a massive, long-term investment for a community. Its design must look ahead to anticipate new medical breakthroughs, potential pandemics, and evolving technology. That means building in modularity and robust infrastructure from day one, ensuring the facility remains a vital asset for decades to come.
For commercial developers and owners, putting money into thoughtful hospital design isn't just another line item on a budget—it's a core strategic investment. A well-designed facility directly leads to better patient safety, higher staff retention, and a much stronger financial position in a fiercely competitive healthcare market.
A Quick Look Back: How We Got Here
To really get a handle on what goes into designing a modern hospital, it helps to understand where we've been. The hyper-efficient, sterile facilities we're familiar with today didn't just appear overnight. They are the product of centuries of trial and error, often sparked by crisis and always chasing better outcomes for patients. The story of hospital architecture is really the story of medicine itself.
It all started back in the 19th century. Hospitals then were often scary places—overcrowded, stuffy, and rife with infection. Mortality rates were shockingly high. It was obvious that something drastic had to change, and that change came in the form of the Pavilion Plan. This wasn't just a new building style; it was a philosophy that treated the building itself as part of the cure.
Think of it like a collection of separate, smaller buildings (the "pavilions") connected by open-air walkways. The genius was in its simplicity: isolate infectious diseases and flood the wards with two of nature's best healers—fresh air and sunlight.
From Open-Air Pavilions to Standardized Towers
The Pavilion Plan was a massive leap forward. First appearing in the 1860s, this design literally saved lives by using natural ventilation to stop germs from spreading between wards. The results were dramatic, with mortality rates in some hospitals dropping from a staggering 30% to less than 10% by the turn of the century. The idea caught on fast; by 1875, more than 200 hospitals across the U.S. had adopted it.
Then, the mid-20th century brought a different set of priorities. After World War II, the name of the game was efficiency. In the U.S., the 1946 Hill-Burton Act poured money into building over 4,600 healthcare facilities. The catch? They had to be "modern," which meant centralized nursing stations and cookie-cutter room layouts designed to make staff workflows as smooth as possible. This is when we started moving away from the sprawling pavilion campuses and toward the compact, vertical hospital towers we see everywhere today. You can find more great historical context on this shift over at Healthcare Design Magazine.
This push for efficiency set the stage for the next major revolution in hospital design—one that would swing the focus right back to the patient.
The Shift to the Single-Patient Room
For a long time, putting multiple patients in a single large ward was just how it was done. It seemed cheaper on paper, but the hidden costs were huge: rampant infections, constant noise, and a complete lack of privacy. Eventually, data from Evidence-Based Design confirmed what common sense already told us: a shared room is a terrible place to recover.
The modern push for single-occupancy, or private, rooms is a fundamental change in thinking. It treats the patient room not just as a bed in a building, but as a critical tool in the healing process itself.
A private room is no longer a luxury amenity. It's a strategic investment with a clear ROI, impacting everything from patient safety and staff efficiency to the hospital's bottom line.
This isn't just a gut feeling; the numbers back it up. Switching to single-patient rooms has been shown to:
- Slash Hospital-Acquired Infections (HAIs). It's simple: fewer people in a room means fewer germs to share, and it makes deep cleaning far more effective.
- Improve sleep and lower stress. By getting rid of the noise and constant interruptions of a roommate, patients can actually rest and heal.
- Boost patient privacy and communication. Patients and their families can have sensitive conversations with doctors without being overheard.
- Increase patient satisfaction scores. In today's value-based care models, happy patients are crucial, as their satisfaction scores are often tied directly to how much a hospital gets reimbursed.
By giving each patient their own space, hospitals create a controlled environment that protects the vulnerable and promotes genuine recovery. This journey from wide-open wards to private rooms tells you everything you need to know about where hospital design is headed: it’s all about building for the individual.
Core Principles of Patient-Centered Design
Patient-centered design isn’t just some feel-good philosophy. It’s a practical, data-backed strategy that treats the physical environment as an active partner in the healing process. The whole idea is to shift away from a purely clinical, process-driven model toward one that puts the comfort, safety, and emotional well-being of patients—and the staff caring for them—first.
Let’s be honest, a hospital can be an intimidating, confusing place. Every single design choice, from the layout of a room to the type of lighting in a hallway, is a chance to lessen that stress.
The thinking here is straightforward: when patients feel safe, respected, and comfortable, their bodies can focus on healing. For developers and owners, this approach creates tangible returns, including shorter hospital stays, fewer medical errors, and better patient satisfaction scores, which are increasingly tied directly to financial reimbursements.
The Power of Single-Occupancy Rooms
If there's one design decision that has a massive impact on modern hospitals, it’s the shift to single-occupancy patient rooms. For decades, multi-bed wards were the norm, but the evidence is now overwhelming—giving patients their own private space is a game-changer. This isn't about luxury; it's a fundamental component of effective infection control and patient recovery.
Moving to private rooms, a trend that really took off after the 2000s, delivers a clear return on investment through improved safety, satisfaction, and day-to-day efficiency.
Let's look at the numbers. When Sutter Health's Eden Medical Center in California was built with 100% private rooms, they saw hospital-acquired infections (HAIs) drop by a staggering 42%. Even more, staff injuries from patient handling fell by 65%, and noise levels dipped by 5-7 decibels, helping patients get much-needed rest.
Across the U.S., hospitals making this switch have seen patient stays shorten by 10-16% and satisfaction scores jump by 20%. These aren't small figures—they translate into millions of dollars in annual reimbursements.
This chart shows just how far hospital design has come, landing on the modern, patient-focused model.
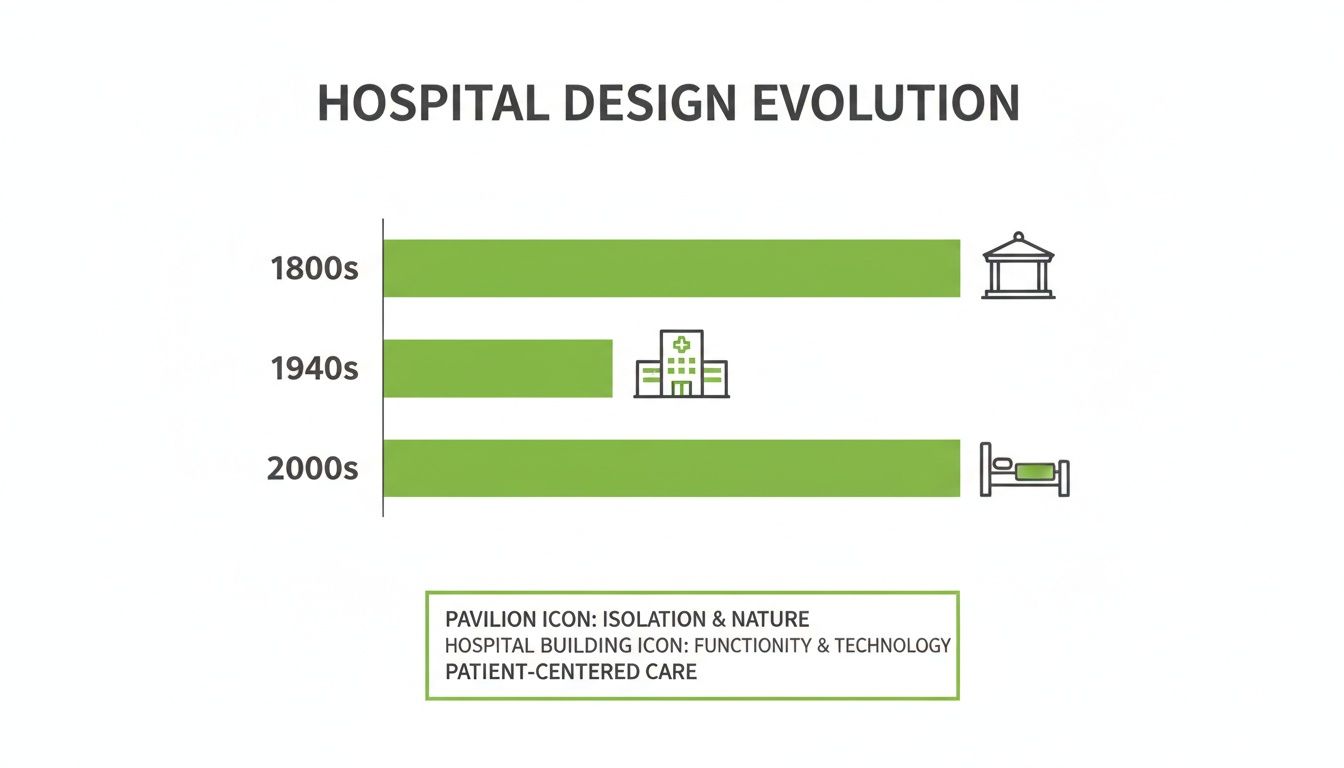
As you can see, the priorities have evolved from just basic sanitation and efficiency to a sophisticated model that puts the individual patient’s experience at the heart of everything.
The contrast between old-school multi-bed wards and modern private rooms is stark, and the data speaks for itself.
Impact of Single-Occupancy vs Multi-Bed Rooms
| Metric | Multi-Bed Ward (Baseline) | Single-Occupancy Room (Improvement) |
|---|---|---|
| Hospital-Acquired Infections (HAIs) | Higher risk of cross-contamination | 40-50% reduction in transmission rates. |
| Patient Satisfaction Scores | Lower due to noise and privacy issues | 20% average increase in HCAHPS scores. |
| Average Length of Stay | Longer recovery times | 10-16% shorter stays, leading to higher bed turnover. |
| Staff Injuries | Higher rates of handling-related injuries | Up to 65% reduction in patient handling injuries. |
| Medical Errors | Increased risk due to distractions | Fewer errors from improved communication and fewer interruptions. |
| Patient Privacy & Dignity | Severely compromised | Fully supported, leading to better patient-doctor communication. |
Ultimately, investing in single-occupancy rooms isn't just a capital expense; it's a strategic investment in better outcomes, lower operational risk, and a stronger financial position for the hospital.
Designing for Staff Efficiency and Safety
A patient-focused design is only half the story. It has to be a staff-focused design, too. A burned-out, stressed, or inefficient clinical team simply can't deliver top-tier care. The hospital's layout can either be a constant source of friction or a powerful tool for boosting workflow and morale.
Think of it like a Formula 1 pit crew, where every tool and every movement is optimized for speed and precision. That’s the kind of thinking we need to apply to hospital design.
By optimizing workflows and reducing physical strain, a well-designed hospital becomes a safer and more efficient workplace. This directly leads to lower staff turnover, fewer errors, and a higher quality of care.
Here are a few key strategies that make a real difference for staff:
- Decentralized Nursing Stations: Instead of one massive, central hub, smaller substations are placed much closer to patient rooms. This simple change dramatically cuts down on the miles nurses walk each shift, freeing up valuable time for actual patient care.
- Clear Sightlines: Smart layouts that give nurses a direct line of sight into patient rooms from hallways or workstations enable passive monitoring. This enhances safety without making patients feel like they’re constantly being watched.
- Ergonomic Design: Every detail matters, from the height of countertops to the strategic placement of patient lifts. These considerations are all about reducing the physical wear-and-tear that leads to costly workplace injuries.
- Staff Respite Areas: It’s crucial to provide dedicated quiet zones—away from the clinical chaos—where staff can decompress and recharge. These spaces are essential for preventing burnout and keeping the team focused and resilient.
Of course, a core part of any patient-centered design is implementing robust safety measures for everyone. This runs the gamut from slip-resistant flooring to highly specialized fixtures in certain environments. For instance, in behavioral health settings, a key focus is on enhancing patient safety with anti-ligature solutions in NHS hospital wards.
At the end of the day, an investment in a design that supports the staff is a direct investment in patient safety and the hospital’s long-term operational health.
Using Nature to Improve Healing and Efficiency

Bringing nature into a hospital isn't just about making the place look nice. It's a strategic, evidence-based approach called biophilic design, and it's a powerful tool for improving health outcomes, boosting staff morale, and delivering a real return on investment.
At its core, the idea is simple: people have an innate need to connect with the natural world. When you fulfill that need within a clinical setting, you can actually speed up the healing process.
This isn't some new fad. The core principles of biophilic design have been around for decades, built on a long-standing understanding of nature's therapeutic power. Today, it’s a non-negotiable part of modern hospital design. Natural light, views of greenery, and even natural materials aren't just amenities anymore—they're necessities that create a calmer, more restorative environment for everyone.
The Proven Link Between Nature and Recovery
The credibility behind this approach is built on a mountain of solid research. The real turning point was a landmark 1984 study by Roger Ulrich, which gave us the first hard proof of what many intuitively knew. His research showed that post-op patients who could see trees from their window recovered faster and needed less pain medication than those staring at a brick wall.
That study essentially launched the "Healing by Design" era, and countless analyses since have backed it up. The data is clear: exposure to nature directly correlates with better health outcomes.
By thoughtfully weaving elements of the natural world into the building itself, a hospital becomes an active participant in the healing process—measurably shortening recovery times and reducing patient stress.
For patients, the benefits are tangible and well-documented:
- Reduced need for pain medication: Exposure to natural light and green views has been shown to lower patients' reliance on analgesics.
- Shorter hospital stays: Patients in rooms with plenty of daylight and nature views are often discharged sooner.
- Lower rates of depression: Natural light helps regulate our internal clocks, which can improve mood and combat feelings of depression and anxiety.
These patient benefits have a ripple effect, leading to higher satisfaction scores and bolstering the facility’s reputation in the community.
The Financial Case for Biophilic Design
For developers, contractors, and hospital administrators, here’s the bottom line: biophilic design pays for itself. The upfront investment in larger windows, healing gardens, or interior green spaces generates substantial, long-term financial returns. It’s a smart business decision, not just an aesthetic one.
This connection between nature and operational efficiency is well-documented. Natural light is now foundational to modern layouts because it delivers proven gains, making it highly attractive to developers focused on hitting energy codes and sustainability goals.
The numbers tell the story. Ulrich's 1984 study found patients with garden views recovered 8.5% faster and needed 22% fewer analgesics. Fast forward to 2023, and 85% of new U.S. hospitals are being built with 20-30% more glazing, leading to measurable drops in infections and stress. Facilities that adopt standards like the WELL Building Standard, which mandate daylight, can see huge energy savings; some have cut costs by $500,000 per year in a single tower just by optimizing window designs. You can explore more global medical trends on WTW's insights page.
The financial upside doesn't stop with energy savings. A work environment filled with natural light and views is proven to reduce staff stress and burnout. In an industry with notoriously high turnover, that translates directly to better employee retention and massive cost savings. A happier, more focused staff also makes fewer errors, which improves patient safety and lowers the risk of costly litigation. When you look at every design choice through a financial lens, biophilic design stands out as a high-impact, high-value strategy.
Designing for Compliance and Future Demands
Once you get past the patient-focused layouts and welcoming lobbies, you run headlong into the non-negotiable world of technical compliance. A modern hospital is one of the most intensely regulated buildings you can possibly build, wrapped in a thick web of codes that dictate everything from safety to patient privacy.
For anyone on the development or construction side, getting this part right isn’t just important—it’s everything. This regulatory framework is the building’s DNA, spelling out the rules for corridor widths, operating room air pressure, and thousands of other details. It's not about checking boxes; it's about building a facility that’s safe, legal, and functional from the moment the doors open.
Navigating the Regulatory Maze
In the United States, the conversation starts with the FGI Guidelines for Design and Construction of Hospitals. Think of these as the industry bible. They aren't just suggestions; most states adopt them directly into law, making them the baseline for the entire physical environment.
But FGI is just one piece of the puzzle. Several other major regulations are just as critical:
- HIPAA (Health Insurance Portability and Accountability Act): Most people think of HIPAA in terms of digital records, but its privacy rules deeply influence physical design. How do you stop sensitive conversations from being overheard in a busy waiting area? You design for acoustic privacy, ensuring exam rooms are properly soundproofed and reception desks are positioned thoughtfully.
- ADA (Americans with Disabilities Act): This federal law demands complete accessibility, which in a hospital setting goes way beyond just adding ramps. It means specifying patient lifts, guaranteeing clear floor space in every bathroom, and making sure counters and equipment can be used by everyone, regardless of their physical abilities.
Don't look at these codes as restrictions. See them as a blueprint for excellence. They give us a standardized, peer-reviewed playbook that ensures every new hospital is built to an incredibly high standard, protecting patients, staff, and the owner’s investment.
The Beating Heart of the Hospital: MEP Systems
If the building’s structure is its skeleton, then the Mechanical, Electrical, and Plumbing (MEP) systems are its vital organs. These incredibly complex networks are the hospital's beating heart, running 24/7 to support life-sustaining functions. It's no surprise they represent a huge chunk of the budget—often 30-40%—and getting them right is paramount.
The HVAC system alone is a perfect example. Understanding the different commercial HVAC system types is fundamental because in a hospital, it’s a primary weapon against infection. These aren’t your typical office building systems. They create negative pressure rooms to contain airborne pathogens and positive pressure suites to shield vulnerable patients in operating rooms.
Then there's the electrical grid, which needs to be designed for 100% redundancy. A power outage isn't an inconvenience; it can be a life-or-death event. This means robust emergency generators and uninterruptible power supply (UPS) systems must be ready to kick in instantly, keeping ventilators, surgical lights, and other critical gear running without a flicker.
Finally, the plumbing network includes a whole separate infrastructure for medical gases. This intricate system of pipes delivers oxygen, medical air, and suction directly to the patient’s bedside, making it as vital as the water supply itself.
Building for Tomorrow: Flexible and Resilient Design
A hospital built today needs to be ready to serve its community for the next 50 years. That’s a long time, and it demands a design that can adapt to new technologies and withstand the unexpected.
Future-proofing is all about designing for change. Instead of building rigid, single-use spaces, the smart move is to use modular components and universal room layouts. A room might be a standard patient room today but could be easily converted into a higher-acuity unit tomorrow with minimal disruption. This is achieved by planning for "soft spaces" (like offices) next to clinical areas for easy expansion and running oversized utility chases to accommodate future wiring and tech.
At the same time, resilient design focuses on keeping the hospital running during a crisis. Think of a natural disaster or a regional blackout. A resilient hospital can essentially become a self-sufficient island, with its own on-site water storage, robust backup power, and a structure built to handle extreme weather. It doesn’t just survive the event—it stays fully operational to care for the community when it’s needed most. This isn't a "nice-to-have" anymore; it's a core expectation.
The Strategic Value of Adaptive Reuse in Healthcare
When we talk about building hospitals, the conversation usually defaults to new, ground-up construction. But there’s a powerful, often-overlooked strategy that savvy developers are turning to: adaptive reuse. This is the art of transforming an existing building—maybe a struggling office complex, an empty big-box store, or even a warehouse—into a state-of-the-art healthcare facility.
For developers and owners, this is more than just a nod to sustainability; it’s a brilliant financial play. Adaptive reuse can slash project timelines by leapfrogging the often-painful entitlement and site prep stages. Buying an existing building is almost always cheaper than acquiring raw land and building from scratch, and you might even qualify for historic preservation tax credits. It's about seeing the untapped potential in a property and turning it into a vital community asset.
Overcoming Unique Design Hurdles
Of course, retrofitting a building for healthcare isn't a simple paint-and-carpet job. It comes with its own set of puzzles that require some serious expertise to solve. The biggest challenge, time and again, is the MEP (Mechanical, Electrical, and Plumbing) systems. A standard office building’s infrastructure just can’t handle the load of a medical clinic. You need specialized HVAC for infection control, dedicated medical gas lines, and beefy electrical systems with robust emergency backup power.
Then there’s the challenge of making the floor plan actually work for a clinical setting. You have to completely rethink a layout designed for cubicles or retail shelves to create smooth, logical pathways for patients and staff. This means creating smart adjacencies—like putting exam rooms near labs—and ensuring every inch meets strict HIPAA privacy rules and ADA accessibility standards.
The core task in adaptive reuse is to surgically insert the complex systems of a modern healthcare environment into the shell of a building designed for a completely different purpose, all while maintaining structural integrity and meeting rigorous codes.
Real-World Applications and Success
The beauty of adaptive reuse is its flexibility. It opens the door to some really creative solutions that meet specific healthcare needs. We see it working successfully all the time in these kinds of scenarios:
- Office Building to Outpatient Clinic: A half-empty suburban office park is a prime candidate. The existing offices can be converted into exam rooms with relative ease, while larger conference rooms make perfect waiting areas or physical therapy gyms.
- Big-Box Retail to Imaging Center: A former "big-box" store offers exactly what you need for an imaging center: vast, open floor plans and high ceilings. This makes it much easier to install bulky equipment like MRI and CT scanners, which have very specific structural and shielding requirements.
- Warehouse to Ambulatory Surgery Center: Warehouses are fantastic for this. Their wide-open, column-free spaces are ideal for laying out operating rooms and sterile processing departments, and their strong frames can easily support heavy equipment and new MEP infrastructure.
At the end of the day, adaptive reuse is a strategy that perfectly marries financial pragmatism with community need. By reimagining our existing buildings, developers can bring essential healthcare services to a community faster and more affordably, breathing new life into old structures and creating incredible, lasting value.
Common Questions About Hospital Design
When you're staring down the barrel of a hospital project, the questions can feel endless. For developers, owners, and contractors stepping into this highly specialized world, a few key questions always seem to pop up. Let's break down some of the most common ones with practical answers to get you started on the right foot.
What Are the Biggest Cost Drivers in Hospital Construction?
Forget what you know about typical commercial builds. In a hospital, the lion's share of the budget—often 30-40%—gets eaten up by the incredibly complex MEP (Mechanical, Electrical, Plumbing) systems. We're not just talking about standard HVAC; this includes sophisticated air handling for infection control, a web of medical gas lines, and a robust electrical grid with non-negotiable emergency backup power.
Beyond the MEP, a few other big-ticket items will drive up your costs:
- Heavy-duty medical equipment is a major factor. Things like MRI or CT scanners are not only expensive on their own, but they also demand serious structural reinforcement and sometimes even radiation shielding built right into the walls.
- Interior finishes have to be tough as nails. Every surface must withstand harsh cleaning protocols and relentless wear while meeting strict infection control standards.
- The building's structure itself needs to be beefier to handle the weight of all that equipment and designed with future changes in mind.
Getting a handle on these expenses early in the design phase is the single best way to keep the budget from spiraling out of control without cutting corners on safety or long-term function.
How Can Design Help a Hospital Adapt to Future Needs?
The secret is thinking in terms of flexibility and modularity. A well-designed hospital isn't a rigid, static monument; it's more like an adaptable platform built to handle decades of unpredictable change.
The real goal here is to create a building that can grow and change right alongside medical technology and community health demands, all without needing a complete—and completely unaffordable—overhaul every few years. That’s how you ensure the building remains a valuable asset for the long haul.
This means using smart strategies like universal room layouts that can shift purpose with minimal effort—turning a standard patient room into a higher-acuity ICU space, for example. It also involves strategically placing "soft space," like administrative offices, next to clinical departments so they can easily expand when needed. Simple but brilliant tactics like using modular wall systems and designing oversized utility corridors for future tech are also game-changers.
What Is the First Step in Planning a Hospital Project?
Before you even think about breaking ground, the most critical step is deep-dive pre-design planning and programming. This is the foundation upon which everything else is built, and getting it right is the best predictor of a successful project.
This phase is all about assembling your core team—architects, engineers, clinical staff, and facility managers—to hammer out the project's goals, scope, and functional needs in painstaking detail. You'll run feasibility studies, analyze the site or existing structure, forecast patient numbers, and map out how every department needs to connect and flow. A rock-solid programming phase is your best insurance against costly changes down the line, ensuring the final building truly works for the healthcare provider.
At Sherer Architects, LLC, we thrive on turning these complex requirements into healthcare environments that are functional, beautiful, and built to last. Whether you're planning a new facility from the ground up, a strategic renovation, or an adaptive reuse project, our team knows how to navigate every stage. We ensure your investment delivers real value for decades to come.
Learn how we can bring structure to your vision at https://shererarch.com.